Studies have found that hypertension is associated with an increased risk of developing MCI. For example, a meta-analysis published in the Journal of Alzheimer's Disease in 2019 that included 14 studies and over 76,000 participants found that people with hypertension had a 26% higher risk of developing MCI compared to people without hypertension. Another study published in the journal Neurology in 2018 found that people with hypertension who also had a higher pulse pressure (the difference between systolic and diastolic blood pressure) had a higher risk of developing MCI compared to those with lower pulse pressure.
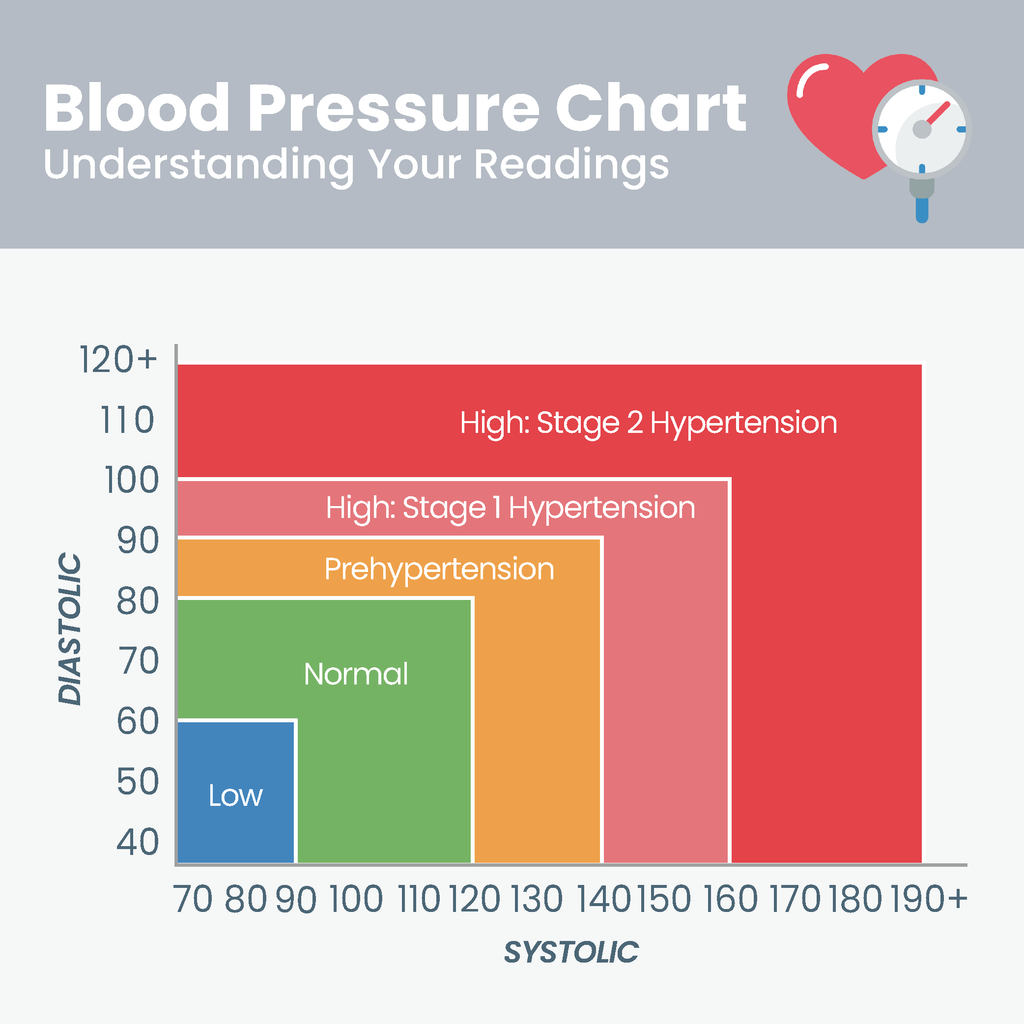
It is believed that hypertension may contribute to the development of MCI through several mechanisms. For example, hypertension can cause damage to the small blood vessels in the brain, leading to reduced blood flow and oxygen delivery to the brain, which can impair cognitive function. Hypertension can also lead to the accumulation of beta-amyloid plaques in the brain, which are a hallmark of Alzheimer's disease and can contribute to cognitive decline.
MCI often involves the same types of brain changes seen in Alzheimer's disease or other forms of dementia. In MCI, those changes occur to a lesser degree. These changes include:
Clumps of beta-amyloid protein, called plaques, and tangles of tau proteins are seen in Alzheimer's disease.
Microscopic clumps of a protein called Lewy bodies. These clumps are associated with Parkinson's disease, dementia with Lewy bodies and some cases of Alzheimer's disease.
Small strokes or reduced blood flow through brain blood vessels.
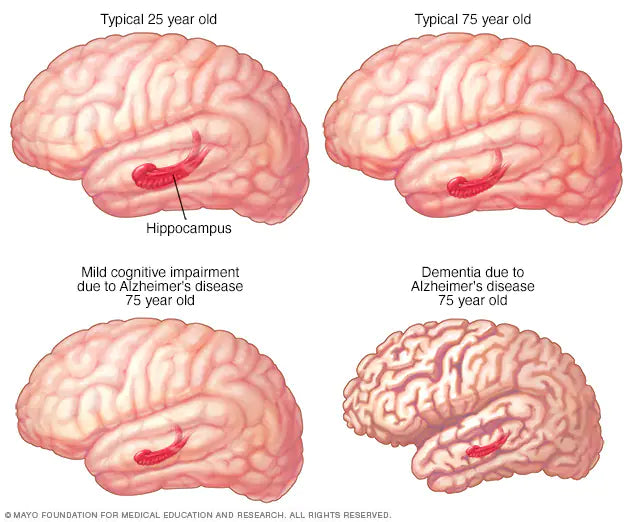
Brain-imaging studies show that the following changes may be associated with MCI:
Decreased size of the hippocampus, a brain region important for memory.
Increased size of the brain's fluid-filled spaces, known as ventricles.
Reduced use of glucose in key brain regions. Glucose is the sugar that's the main source of energy for cells.
The strongest risk factors for MCI are:
Increasing age.
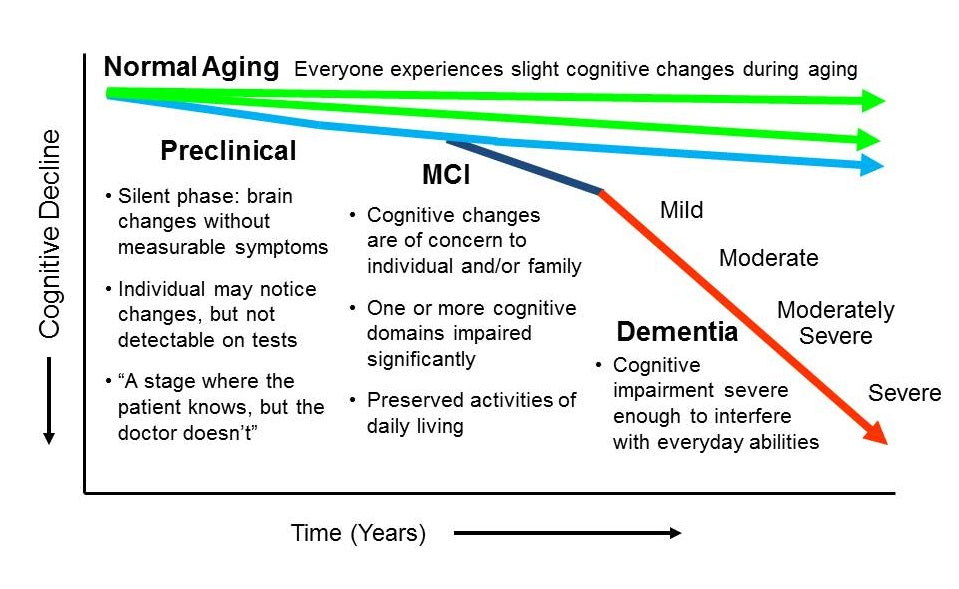
Having a form of a gene known as APOE e4. This gene also is linked to Alzheimer's disease. But having the gene doesn't guarantee that you'll have a decline in thinking and memory.
Other medical conditions and lifestyle factors have been linked to an increased risk of changes in thinking, including:
Diabetes
Smoking
High blood pressure
High cholesterol
Obesity
Depression
Obstructive sleep apnea
Lack of physical exercise
Low education level
Lack of mentally or socially stimulating activities
Complications
People with MCI have an increased risk — but not a certainty — of developing dementia. Overall, about 1% to 3% of older adults develop dementia every year. Studies suggest that around 10% to 15% of people with MCI go on to develop dementia each year.

Managing Hypertension to Reduce the Risk of MCI:
Mild cognitive impairment can't be prevented. But research has found some lifestyle factors may lower the risk of getting MCI. Studies show that these steps may help prevent MCI:
Don't drink large amounts of alcohol.
Limit exposure to air pollution.
Reduce your risk of a head injury.
Don't smoke.
Manage health conditions such as diabetes, high blood pressure, obesity and depression.
Practice good sleep hygiene and manage any sleep problems.
Eat a healthy diet full of nutrients. Include fruits and vegetables and foods low in saturated fats.
Stay social with friends and family.
Exercise at a moderate to vigorous intensity most days of the week.
Wear a hearing aid if you have hearing loss.
Stimulate your mind with puzzles, games and memory training.
Conclusion:
Hypertension is a significant risk factor for MCI, a condition characterized by a decline in cognitive function that is greater than expected for an individual's age and education level. People with hypertension should work closely with their healthcare providers to manage their blood pressure and reduce their risk of developing MCI. This may involve lifestyle changes such as a healthy diet, regular exercise, and stress management, as well as medications to help lower blood pressure. By taking these steps, people with hypertension can reduce their risk of cognitive decline and improve their overall quality of life.


Leave a comment
This site is protected by hCaptcha and the hCaptcha Privacy Policy and Terms of Service apply.